We here at Flex® love consensual sex in every form (Don’t believe us? See here, here, and here to learn more 😉). It’s a mood booster, it releases endorphins, and it can even help reduce period cramps.
All good things. However: On the rare occasion, sex can have other, not-so-desirable effects on our bodies. Unexpected bleeding is one possibility.
Ever snuck out to pee after sex (which is a very good call, BTW) and noticed a few drops of blood on your TP? Or found an unexpected streak of blood on your sheets after waking up the next morning? Depending on the timing, it could be your period—but bleeding during or after sex can happen for a number of other reasons, too.
If you’ve triple-checked your period tracker app and ruled out menstruation as a possibility, those drops of blood could be something as innocent as a little bit of vaginal tears due to rougher-than-usual sex (we’re all for it, but don’t hold back on the lube!). However, they could also be an early indication of a more serious condition—and this is why it’s so important to report any instances of postcoital bleeding to your health care provider.
Here’s what you need to know about bleeding during or after sex, including when to talk to a doctor, risk factors, what sort of bleeding is “normal,” and what other symptoms to look out for.
Why am I bleeding after sex? Common causes
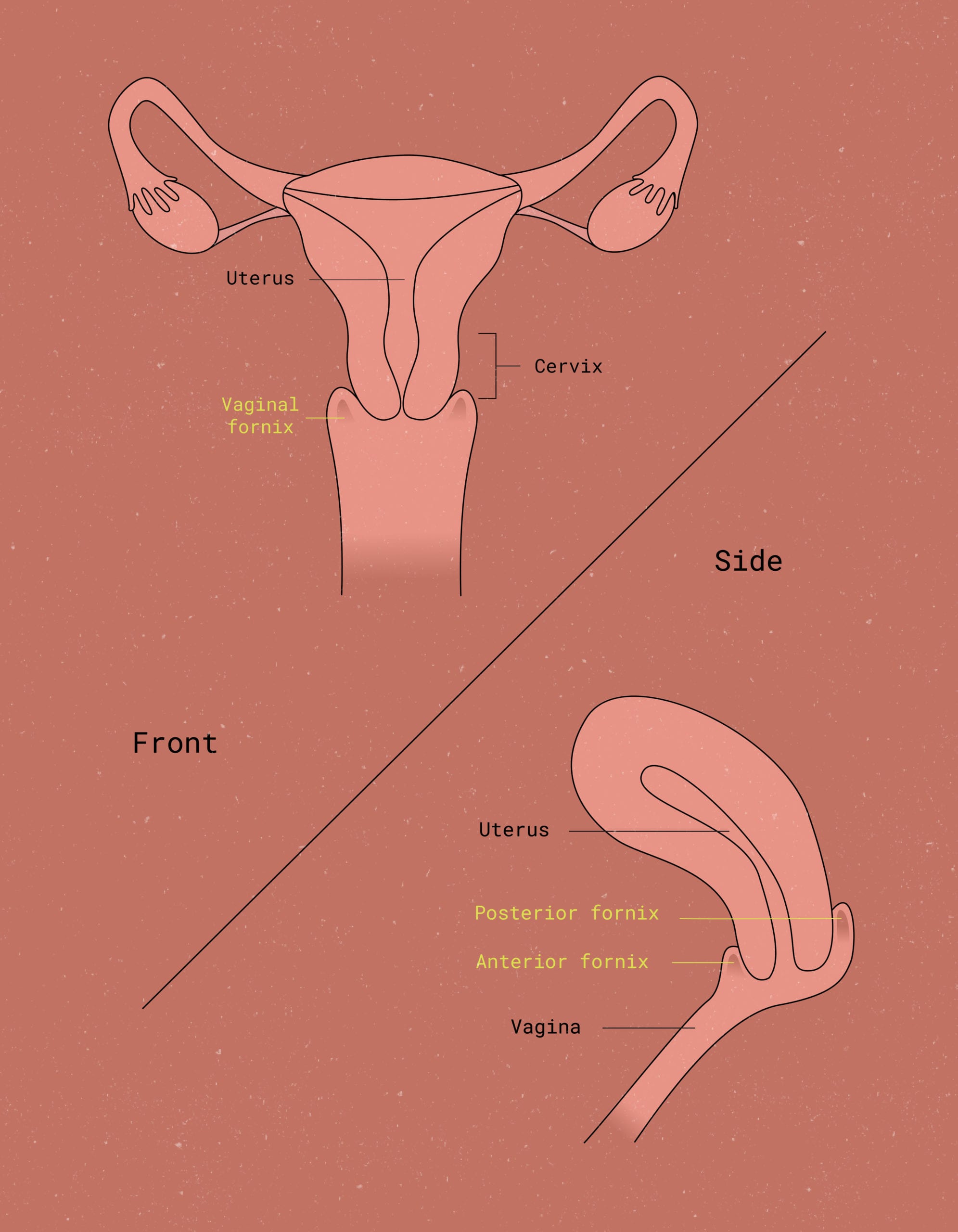
We’ve said it before, and we’ll say it again: Pay attention to your vagina! It can tell you more about your underlying health than you might think.
Anything that’s noticeably outside the norm for you—and, remember, this might not be the same as the “norm” for your best friend—is worth bringing up to your PCP or healthcare provider. This includes bleeding when you wouldn’t typically expect it.
If you’re not on your period, possible causes of postcoital bleeding can include various reproductive system issues. Some of the conditions that could cause you to bleed during or after sex include:1 2
- Vaginal atrophy or vaginal dryness
- Perimenopause
- Trauma to the vagina or cervix
- Friction (due to a lack of moisture or foreplay)
- Vaginal infections, including certain STIs (chlamydia trachomatis, gonorrhea, pelvic inflammatory disease (PID), trichomoniasis)
- Genital sores (such as those brought on by genital herpes or syphilis)
- Cervicitis (inflammation of the cervix)
- HPV
- Vaginitis
- Cervical ectropion
- Endometrial (uterine) or cervical polyps
- Uterine fibroids
- Uterine prolapse
- Cervical or endometrial (uterine) cancer
While many of the above conditions are treatable or relatively benign, it’s important to note that post-sex bleeding is one of the first symptoms of cervical cancer. About 11% of people with cervical cancer experience some bleeding during or after sex with penetration.3
Don’t panic, though: The prevalence of cervical cancer has gone down in recent years, largely thanks to the uptick in screening. Just make sure you’re getting regular Pap tests and pelvic exams.
Some blood during or after sex isn’t uncommon if you’re having rough sex or if you tend to experience vaginal dryness (or a combination of those two factors). Also, keep in mind that bleeding or light spotting is pretty common after your first time having penetrative sex—or even your first couple of times. This happens as a result of the tearing or stretching of the hymen.
What if it really is your period?
It’s not unheard of to start your period a bit sooner than you expected after having sex—but when we say “a bit sooner”, we mean by a couple of days, and not a whole week or more. If your period was already scheduled to arrive, having sex that ends in an orgasm (the orgasm being the key factor at play here) could theoretically kick-start the uterine contractions that speed up the shedding of your uterine lining.
Nothing is more of a buzz-kill than unexpectedly staining the sheets when your period arrives mid-sesh. But don’t let a little blood stop you from having fun: Try a menstrual disc, like Flex Disc, next time you’re on your period and have all the mess-free period sex your heart desires. Want to learn more about having sex with a menstrual disc? Read all about it here.

When to see a doctor about bleeding during sex
As with most things that have to do with your reproductive and sexual health, you’re better safe than sorry. Unless you are absolutely certain that the blood you noticed after your most recent romp between the sheets was really your period, you should mention it to your gynecologist or healthcare provider—ASAP.
If possible, take note of the amount of blood, what day of your menstrual cycle you were on, and where the blood seemed to be coming from. Try to relay as much detail as possible, for example, if you bleed after sex with no pain or if it is painful during or after intercourse. Your provider will likely perform a physical exam such as a pelvic exam and may recommend additional testing (for example, a Pap smear, sexually transmitted infection or STI screen, or biopsy) to check for underlying conditions.3
Other symptoms to look out for include:
- Unusual vaginal discharge
- Unusual or foul vaginal odor
- Pain during sex
- Pelvic pain
- Painful urination
- Flu-like symptoms or fever
- Abnormal, painful, irregular, or unusually heavy periods
If any of the above apply to you, make sure to mention them to your healthcare provider in addition to describing the nature of the postcoital bleed you’ve been experiencing. The sooner you get a diagnosis, the better—even if that diagnosis ends up being something totally harmless, like vaginal dryness.
The only time you’re off the hook for that chat with your doctor? If you’re 100% sure it was your period or if it was your very first time having penetrative sex, you can skip it (for now). In those cases, do keep an eye out for unexplained bleeding the next time you have sex, and if it happens, you know what to do.
Bleeding during sex vs. postcoital bleeding: Does the timing matter?
Healthcare professionals typically put non-menstrual bleeding that happens either during sex or after sex into the same category.2 The exact timing isn’t important. You might be a little bit too distracted to notice exactly when those first drops of blood were shed, anyways—so don’t stress if you can’t pin down those details.
We will note, however, that vaginal bleeding after sex can sometimes be confused with blood coming from other areas, such as the urinary tract (which could signal a UTI or other bladder infection) or the rectum. A small mirror and a clean tissue can come in handy when identifying exactly where the blood is coming from—but if you can’t tell, no worries. Just keep your provider in the loop and take note of any other symptoms (like burning when you pee or unusual odor).
How to prevent bleeding during or after sex
If you’ve talked to your doctor and you’ve determined that your post- or mid-sex blood is not due to an underlying condition, but simply due to friction and/or vaginal dryness, there are a few steps you can take to prevent it.
Firstly: Don’t skip the foreplay! Take your time warming up your body and exploring your partner’s, while you’re at it. Kissing, touching, or even introducing a toy for a few minutes longer than usual will give your body time to produce the natural vaginal lubrication that makes sex all the more enjoyable.
If your body has a tougher time getting into WAP mode—which can happen as a side effect of certain medications, as the result of a hormonal imbalance, or when approaching or in the midst of menopause—break out some body-safe lube.
K-Y Jelly is a reliable choice, but there are now many other options available, including newer brands offering vaginal lubricants with CBD. CBD is a natural compound that may enhance pleasure and alleviate pelvic pain for individuals with dyspareunia, although these benefits are not scientifically proven.
Low estrogen to blame? Your provider may be able to prescribe a cream or pill to help boost your hormone levels and help your body produce more of its own lubrication.3

Postcoital bleeding in unique circumstances: With an IUD, during pregnancy, or after menopause
BLEEDING AFTER SEX WHEN YOU HAVE AN IUD
Sometimes after insertion, hormonal IUDs can cause breakthrough bleeding. This is especially common during the first 2-6 months following placement. It’s important to mention that any type of hormonal birth control can cause some spotting after intercourse.
If you have a hormonal IUD (e.g., Mirena, Kyleena, Skyla), light bleeding or spotting during or after sex is common. It usually resolves on its own but contact your provider if it persists beyond a few hours.4
Sidenote: If you have the copper IUD and you notice some blood after sex, you should call your healthcare provider immediately. They will probably want to verify that the device hasn’t been dislodged or bumped out of place. While uncommon, IUD displacement can lead to bleeding and may require urgent medical care.5
BLEEDING AFTER SEX WHILE PREGNANT
Bleeding during pregnancy can be frightening but is fairly common, happening in 15-25% of pregnant people. While most occur in the first trimester, it can happen at other times for various reasons—some harmless, others concerning.6
If you notice light to medium bleeding during or after intercourse while pregnant, it could simply be due to the fact that the cervix becomes more tender and vascular during pregnancy. These cervical changes are normal and nothing to worry about.
The American Pregnancy Association recommends that pregnant individuals talk to their doctor before having penetrative sex again if they notice any blood loss. This is mainly to prevent further irritation.7
Vaginal bleeding after sex during pregnancy could signal a miscarriage or ectopic pregnancy. Heavy bleeding over an extended period is more common in miscarriages, while light spotting is typically not alarming. (P.S. Normal sexual intercourse does not cause miscarriages.)
Lastly, some vaginal bleeding could be a sign of implantation if it’s very early in your pregnancy—within the first six to 12 days after fertilization. Implantation bleeding is believed to happen when the fertilized egg attaches to the lining of the uterus. It doesn’t happen to everyone, but if timing coincides, you might experience light bleeding after sex, as a result. If you suspect you might be pregnant, this might be a good time to get that pregnancy test done.
Here’s the general rule of thumb: If the bleeding is light and takes place during the first half of your pregnancy, you probably don’t need to contact your doctor or OB/GYN.
If the bleeding is medium to heavy, or if you experience even a small amount of blood during the second half of your pregnancy, give your provider a call. They will likely check you for placenta previa or placental abruption, both high-risk conditions that may develop later in pregnancy.
POST-MENOPAUSAL BLEEDING AFTER INTERCOURSE
Postmenopausal people experiencing bleeding during or after sex should contact their healthcare provider immediately. Any vaginal bleeding post-menopause is abnormal and requires further tests done to rule out potential issues, such as benign polyps or cervical/uterine cancer.8
If an underlying cause or medical condition has been ruled out but you are still experiencing abnormal bleeding during or after sexual activity, decreased estrogen levels could be to blame. Lack of estrogen tends to correlate and appears one of the causes of vaginal dryness. In addition, as you age, the tissue of your vulva and vaginal walls begins to thin out. This thinner, more sensitive vaginal tissue is more prone to tearing or abrasion, so make sure to use plenty of lube to avoid bleeding with sex.
What is the best way to stop vaginal bleeding after sex?
If you bleed after sex, it is important to first consult with a healthcare professional to determine the cause. They can provide appropriate advice and treatment options based on your medical history and individual situation. Self-treatment may not be effective or safe in all cases.
If you experience bleeding after sex, available treatments depend on the underlying cause. Common approaches include addressing vaginal dryness with lubricants, treating infections with antibiotics, managing cervical polyps with minor procedures, or adjusting certain medications. It is important to speak with your physician to determine the right treatment for your specific situation.
Is it normal to bleed after sex? Key takeaways
We’ll say it louder for the seats in the back: When in doubt, reach out! Unexpected vaginal bleeding shouldn’t be taken lightly, and that includes during or after sex (when you know it isn’t your period). There are a few exceptions, of course—like if it’s your first time having penetrative sex, or if you’ve just had an IUD inserted—but we’d rather you err on the side of caution.
If you’ve talked to a healthcare provider and already know it’s just good ‘ol friction to blame, it might be a good idea to invest some more time into foreplay the next time you hop in the sack and consider adding a water-based lubricant to the mix (and don’t be afraid to apply with a heavy hand!).

This article is informational only and is not offered as medical advice, nor does it substitute for a consultation with your physician. If you have any gynecological/medical concerns or conditions, please consult your physician.
© 2025 The Flex Company. All Rights Reserved.
- Vaginal bleeding causes. (2019, April 23). Mayo Clinic. https://www.mayoclinic.org/symptoms/vaginal-bleeding/basics/causes/sym-20050756[↩]
- Postcoital bleeding: A review on etiology, diagnosis, and management. (n.d.). PubMed Central (PMC). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4086375/[↩][↩]
- Do you bleed after sex? When to see a doctor. (2021, March 4). Health Essentials from Cleveland Clinic. https://health.clevelandclinic.org/what-should-you-do-if-you-bleed-after-sex/[↩][↩][↩]
- What you should know about breakthrough bleeding with birth control. (n.d.). ACOGACOG stands for the American College of Obstetricians and Gynecologists (a professional membership organization for obstetrician–gynecologists).. https://www.acog.org/womens-health/experts-and-stories/the-latest/what-you-should-know-about-breakthrough-bleeding-with-birth-control/[↩]
- Copper IUD (ParaGard). (2020, February 11). Mayo Clinic – Mayo Clinic. https://www.mayoclinic.org/tests-procedures/paragard/about/pac-20391270[↩]
- Bleeding after sex while pregnant: Possible causes & when to call a doctor. (2020, August 21). What to Expect. https://www.whattoexpect.com/pregnancy/sex-and-relationships/bleeding-after-sex-during-pregnancy/[↩]
- Bleeding during pregnancy. (2021, July 16). American Pregnancy Association. https://americanpregnancy.org/healthy-pregnancy/pregnancy-complications/bleeding-during-pregnancy/[↩]
- O’Connor, A. (2020, August 21). Bleeding after menopause could be a problem. Here’s what to know. ACOGACOG stands for the American College of Obstetricians and Gynecologists (a professional membership organization for obstetrician–gynecologists).. https://www.acog.org/womens-health/experts-and-stories/the-latest/bleeding-after-menopause-could-be-a-problem-heres-what-to-know[↩]