Breakthrough Bleeding: Here’s what you need to know
Everything you need to know about contraceptives & breakthrough bleeding
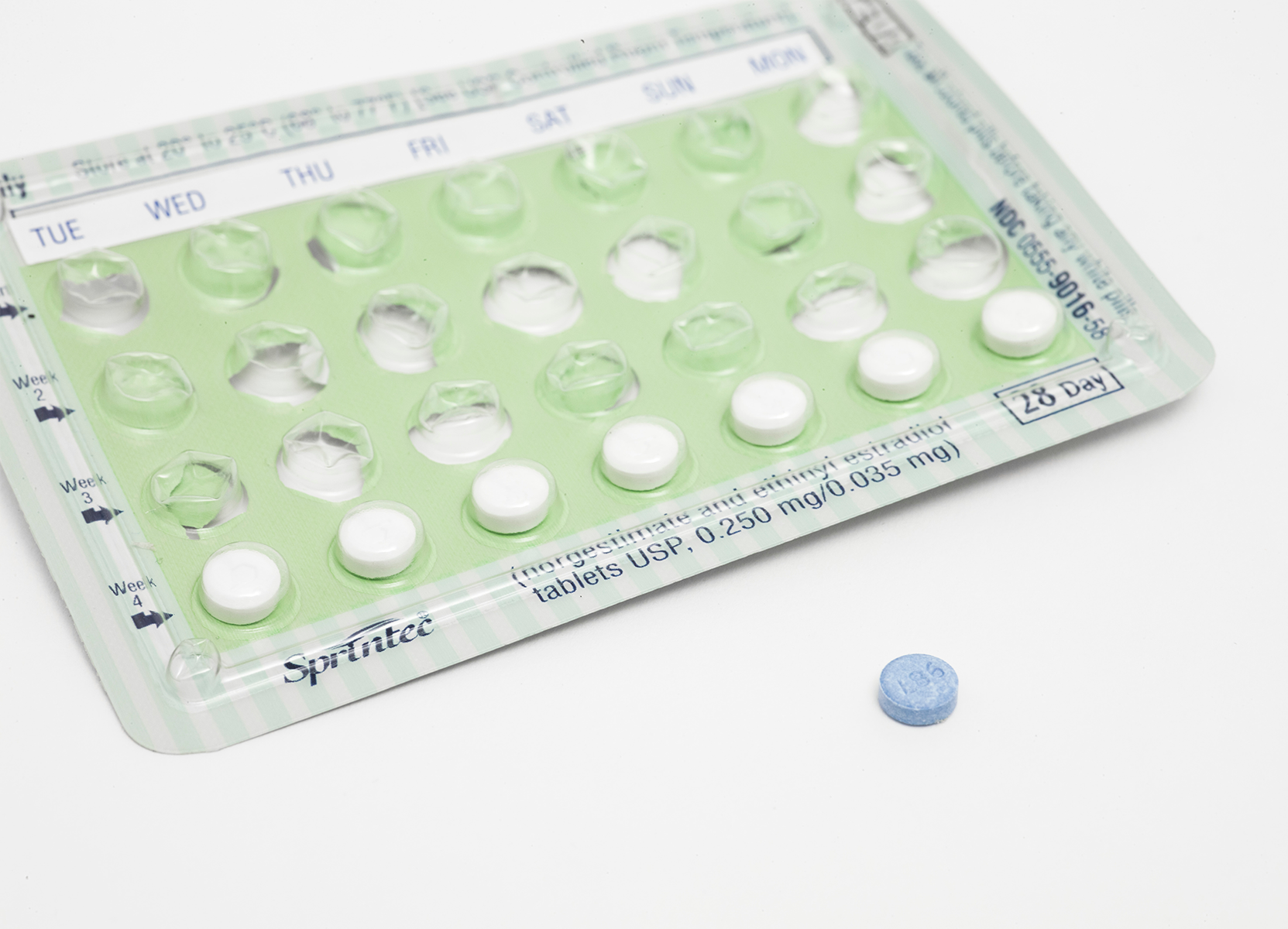
TL/DR: Knowing the facts about birth control bleeding is so important for choosing your contraceptive method. The pill, IUD, and vaginal ring are three of the most common birth control methods. Each method has its own effect on how you bleed.
From the pill to the IUD to the vaginal ring, birth control options have definitely changed over time.
With so many options available, it can be difficult to choose a birth control (BC) method. This is because it can be challenging to remember all the details. This is especially true when it comes to questions such as: How will this affect my period? Does birth control stop your period?
The short answer is this: You may or may not continue to get your period on birth control. It all depends on how your body interacts with the specific kind of contraceptive you choose.
Menstruation vs. breakthrough bleeding vs. withdrawal bleeding: What’s the difference?
With so many terms used to describe how we bleed, let’s start out with a few basic definitions. Your period when not on birth control is different than when on birth control. Most forms of birth control cause different bleeding than natural menstruation.
Menstruation (aka your period)
Refers to your mensesAnother term for menstrual flow (commonly known as your period).. This is the cyclical bleeding that happens with the shedding of the uterine lining. 1
After ovulation, when fertilization does not occur, progesterone levels stay low, allowing the lining of your endometrium to slough off. Your period will usually last for 3 – 7 days and occurs on a roughly monthly time cycle. To learn more about this, we recommend reading Your Cycle article.
Withdrawal bleeding
Is a type of bleeding that happens when your body is no longer being influenced by external hormonal stimulation. You can experience withdrawal bleeding as a result of the withdrawal of those hormones and your body adjusting to new hormone levels. This withdrawal allows the lining of the uterus to shed to produce your period. 2
However, withdrawal bleeding isn’t technically the “same thing” as your period. This is because it happens as the result of the hormonal birth control and not your natural hormonal fluctuations.
In practical terms, withdrawal bleeding occurs during the placebo pill phase of your pill pack. If you use a vaginal ring, during the week when you remove your vaginal ring.
Breakthrough bleeding or spotting
While on pill, is the bleeding that happens in between normal menstrual periods.3 Although it can be annoying and frustrating, it doesn’t generally mean that there’s something abnormal happening down there. Certain factors can increase the likelihood of episodes of bleeding between periods – including some types of birth control.
For example, breakthrough bleeding is more common when you start taking hormonal contraceptive pills. Around 30-50 percent of people experience it during the first 3 to 6 months of being on a new combined pill.4 It usually decreases as your body becomes accustomed to the hormones over the first year. However, a small percentage of people may still experience breakthrough bleeding.
The general thought in the contraceptive community is that birth control with lower doses of estrogen are more commonly associated with breakthrough bleeding. Low dose birth control pills come in two forms. Combination pills use both estrogen and progestin, but provide lower doses of estrogen than traditional pills. Progestin-only pills only contain synthetic progesterone. However, they can work differently for every person.
Other factors that are associated with breakthrough bleeding? Smoking, taking meds that interact with BC, and digestive woes like diarrhea and vomiting that affect absorption of the pill. Missed pills or not taking the pill at the same time every day will also increase the chances of breakthrough bleeding.
The contraceptive ring is also associated with an increased rate of breakthrough bleeding, especially in the first couple months of use. Again, this varies from person to person.
Experiencing bleeding or spotting on birth control? Make note of it in your phone or cycle tracking app of choice. Write down the quantity and appearance, from spotting, a small amount of blood to a full-on bleed, duration, and where in your cycle it happened. Look at your birth control packaging to find the specific day, if you’re having a period during the active pills.
You should always feel comfortable bringing up irregular bleeding patterns to your healthcare provider. Giving as much information as possible is always a good strategy.

How different types of birth control can impact your period
Some of the common types of birth control that we’ll talk about include the oral contraceptive pill, IUD, patch, and the ring. There isn’t only one type of pill available, and calling it “the pill” is a misnomer.
In fact, there are hundreds of types of birth control pills: ones that are estrogen-dominant, progestin-dominant, progestin-only pills(aka minipill). There’s also the ones that have the same dose per day or change throughout the month. And with each of these comes a change in how it does or does not affect your period.
Types of birth control that (might) stop your period
Aside from preventing pregnancy, some types of birth control may also be able to lighten your period. These types are often prescribed for those with health conditions like endometriosis uterine fibroids, PCOS, or even plain old menorrhagia.
These include most forms of combined oral contraceptives the hormonal IUD, and other options like the patch, shot, birth control implant, and ring.5
Depending on the dosage and your body’s own reaction to the contraceptive, these options may also stop your period altogether.
Some people may prefer a form of birth control that stops their period completely. This could be due to the demands of their profession or because of severe menstrual pain. Keep in mind that everyone’s body interacts with birth control differently. Talking to your OB-GYN is the best way to determine which method suits your unique needs.
Stopping/lightening your period with the pill or ring:
There are several specific formulations of the pill, in particular, that are designed to stop your period. These are termed “continuous use” contraceptive pills.
Continuous birth control pills work by “skipping” the normal placebo week in your pack. This provides a consistent inflow of estrogen/progestin that prevents the withdrawal bleeding mentioned above. This is equivalent to not removing the vaginal ring during the fourth week of your cycle.

Stopping/lightening your period with an IUD:
There are two categories of IUDs approved for use in the United States: hormonal and non-hormonal. Hormonal IUDs such as Kyleena, Liletta, Mirena, and Skyla are pretty variable in terms of their impact on your cycle. Things generally even out around the 6-month mark.
Most people with hormonal IUDs will experience lighter and shorter periods over time, although this can vary from person to person. For certain individuals, hormonal IUDs result in no period whatsoever (after the initial adjustment phase). Certain types of hormonal IUDs may also stop periods altogether (amenorrheaThe absence of menstruation, often defined as missing one or more menstrual periods. ), although this is a discussion to have with your provider.
The non-hormonal, copper IUD will not result in a lighter period and, in most cases, does the opposite. Finally, it’s important to note that all IUDs require a visit with a medical provider for insertion and removal. They are an effective long-term contraceptive. However, if you are planning to become pregnant soon, this is something to keep in mind.
Other options: The shot, implant, or patch:
There are also several other BC options that are less frequently talked about in the mainstream. These include the depo-provera birth control shot, the implant, and the patch. All three work differently and have varying pros and cons depending on your unique needs.
These options, in general, will cause lighter periods and may even result in no period for some. Speak with your health care professional to learn more about other options and their side effects.
Curious about the effectiveness of these birth control options? Here’s a helpful infographic infographic straight from the American College of Obstetricians and Gynecologists (ACOGACOG stands for the American College of Obstetricians and Gynecologists (a professional membership organization for obstetrician–gynecologists).)
Heavy bleeding on birth control
Some BC options might do the opposite of what we discussed above – and may actually result in heavier menstrual bleeding. If you had a light period to begin with, this may be no big deal. It may not outweigh the benefits these forms of BC could offer.
The most famous of this category is the non-hormonal copper IUD, the brand name of which is Paragard®. This contraceptive works by creating an environment so toxic to sperm that the odds of fertilization are less than 1 percent. 6
It’s a trade-off. The copper IUD is considered one of the most effective forms of contraception, and it’s low-effort. Insert it once and it lasts for up to 10 years. The other side of the coin is a potentially heavy menstrual flow that may come with some other symptoms.

When to worry about heavy bleeding or breakthrough bleeding on birth control
The first couple of months of any new form of BC can result in changes to your menstrual cycle. These changes can include heavy menstrual bleeding or breakthrough bleeding. Most of this should balance out within about six months or sooner.
It’s important to remember that the copper IUD, in particular, is associated with heavier menstrual bleeding. So, for most people this will be par for the course.
Still experiencing heavy vaginal bleeding while on birth control past the six-month mark? If you are not on the copper IUD, speak with your doctor. Heavy bleeding, FYI, is defined as using more than one pad or tampon an hour on average, bleeding that totals 80mL/5.4 tablespoons or more, and/or bleeding that lasts longer than 7 consecutive days.7
Your healthcare provider will take the necessary measures to ensure that there is not an underlying issue causing your symptoms. Or maybe change to a method that works better for your body.
Birth control bleeding is different for everyone
Not to sound like a broken record, but it’s SO important to remember that your body is unique. This means that your menstrual cycle, and your reaction to different forms of birth control – will vary depending on different factors. Factors include your baseline hormonal levels, comorbidities (e.g. other health conditions), etc.
This means that, although we have population-level data on many if not all of the contraceptive options available, this information represents a bird’s-eye view. So, not all of it is necessarily applicable to YOU as an individual. For this reason, it’s important to communicate with your healthcare provider about your needs prior to beginning any contraceptive regimen.
Ask yourself these questions:
- Are you more concerned about efficacy or ease of use?
- Do you prefer hormonal or non-hormonal methods of birth control?
- Are you interested in potentially becoming pregnant in the short term, or within a couple of years?
- Do you have any pre-existing reproductive or pelvic conditions?
- What cycle-related symptoms (like acne, severe cramps, or headaches) are you experiencing currently that you would like to address

Birth Control Bleeding: Key Takeaways
The more detailed information you give your provider, the better chance you’ll have at finding your ideal BC option, ASAP.
Each method will have its pros and cons and it’s ups and downs with use. Allow your body some time to adjust. Don’t expect perfection in the first week, it may take a month or more.
Understanding your priorities and how contraception fits into your lifestyle is a great start. With that, you can support your provider in presenting options that will align with these needs.
Bleeding will also be a component of this conversation. Some folks prefer a lighter period or no period at all, while others will prioritize a non-hormonal contraception method above others. Some others like the regularity of having a period (or withdrawal bleeding) every month. Your preference is your preference, and you deserve to have this validated by a healthcare provider, with all the available options.
This article is informational only and is not offered as medical advice, nor does it substitute for a consultation with your physician. If you have any gynecological/medical concerns or conditions, please consult your physician.
© 2025 The Flex Company. All Rights Reserved.
- Mayo Clinic Staff. (2019, June 13). Menstrual cycle: What’s normal, what’s not. Mayo Clinic. Retrieved December 02, 2020, from https://www.mayoclinic.org/healthy-lifestyle/womens-health/in-depth/menstrual-cycle/art-20047186[↩]
- Wright, K. P., & Johnson, J. V. (2008). Evaluation of extended and continuous use oral contraceptives. Therapeutics and clinical risk management, 4(5), 905–911. https://doi.org/10.2147/tcrm.s2143[↩]
- Wouk, N., & Helton, M. (2019). Abnormal Uterine Bleeding in Premenopausal Women. American family physician, 99(7), 435–443.[↩]
- Villavicencio, J., & Allen, R. H. (2016). Unscheduled bleeding and contraceptive choice: increasing satisfaction and continuation rates. Open access journal of contraception, 7, 43–52. https://doi.org/10.2147/OAJC.S85565[↩]
- Davies, J., & Kadir, R. A. (2017). Heavy menstrual bleeding: An update on management. Thrombosis research, 151 Suppl 1, S70–S77. https://doi-org.idm.oclc.org/10.1016/S0049-3848(17)30072-5[↩]
- Mayo Clinic Staff. (2020, February 11). Copper IUD (ParaGard). Mayo Clinic. Retrieved December 02, 2020, from https://www.mayoclinic.org/tests-procedures/paragard/about/pac-20391270[↩]
- Sriprasert, I., Pakrashi, T., Kimble, T., & Archer, D. F. (2017). Heavy menstrual bleeding diagnosis and medical management. Contraception and reproductive medicine, 2, 20. https://doi.org/10.1186/s40834-017-0047-4[↩]