The quick highlights:
- A menstrual disc sits in the vaginal fornix, at the base of your cervix, which is the widest part of your vagina; a menstrual cup sits lower, in the vaginal canal
- Discs have a flat, bowl-like shape. Cups have a bell shape with a stem
- Both discs and cups collect period blood, rather than (like a tampon) absorbing it
- Discs are held in place by your pubic bone; cups use light suction against the vaginal walls
- Cups are always reusable; discs come in reusable or disposable (single-use) versions
- Research found menstrual discs have the highest capacity of any period product tested, averaging 61 mL versus 20-50 mL for tampons, pads, and cups 1
- Flex Cup’s patented pull-tab removes without suction, which may reduce IUD expulsion risk (a concern with traditional cups); discs use no suction at all 2
The full read:
Calling a menstrual disc and a menstrual cup the same product would be like equating eyeglasses to contact lenses. Sure, both correct your vision, but they’re entirely different products used in different ways.
Both period cups and period discs are designed to collect menstrual fluid rather than absorb it. But their shapes, placement in the body, and mechanisms are quite different. Below, we break down everything you need to know: how they work, how they’re inserted, what they’re made from, how they compare on capacity, and which activities you can do with each.
Which is better: menstrual disc or cup?
Neither product is objectively better than the other. It depends entirely on your body, your flow, and your lifestyle. Discs tend to offer higher capacity, period-sex compatibility, and no suction. Cups are typically more widely available in multiple sizes, have a longer reusable lifespan, and feel more familiar to tampon users in terms of placement.
Read on for the full breakdown so you can decide which is the better choice for you.

Period cup vs. disc: placement in the body
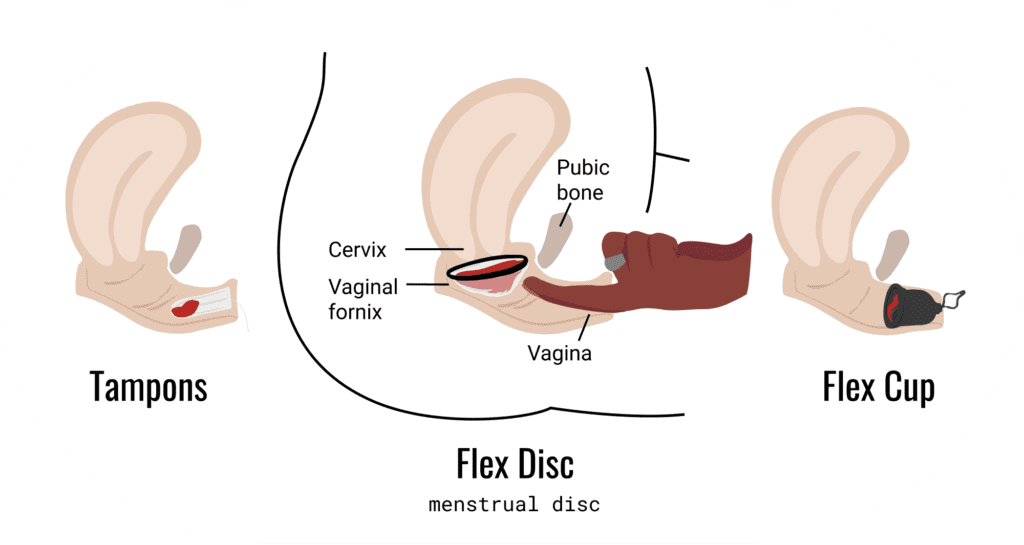
A menstrual disc sits in the vaginal fornix, , the space at the very end of the vaginal canal that cups around the base of your cervix. Because this is the widest part of your vaginal anatomy, discs are wider and flatter than cups.
A menstrual cup sits in the narrower, lower portion of the vaginal canal, below the cervix. If you’re familiar with tampons, cups and tampons occupy roughly the same position, though with a cup you have more control over exactly how far up to place it, since you use your fingers rather than an applicator.
One key anatomical difference worth knowing: the vaginal canal contains more nerve endings than the fornix. This is thought to be one reason many users report that discs feel more comfortable to wear, particularly during the first few cycles of learning.
How do they work? Different mechanisms for disc vs. cup
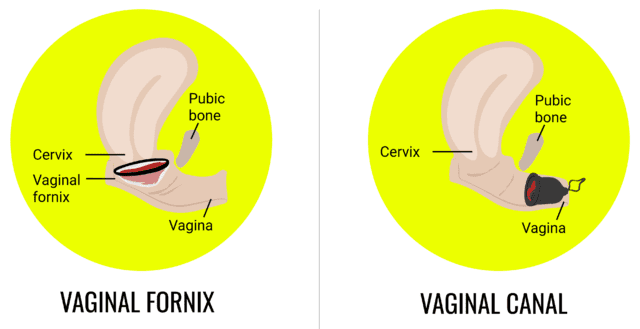
How does a menstrual disc stay in place?
A disc doesn’t use suction. Instead, it’s held in place by the structure of your anatomy. Once inserted, the back rim of the disc rests in the posterior fornix (behind the cervix), and you tuck the front rim up and behind your pubic bone with a finger. Your pubic bone acts like a shelf, keeping the disc stable during wear.
To remove a disc, you hook your finger around the front rim, gently “untuck” it from behind the pubic bone, and carefully pull it out, keeping it as level as possible to avoid spillage.One useful feature of menstrual discs: many users are able to “auto-dump” or “self-empty” their disc while using the bathroom. Because of where the disc sits, bearing down slightly (like you would during urination or a bowel movement) can cause the disc to tilt and release fluid into the toilet without requiring full removal. This can be especially helpful on heavier flow days.
How does a menstrual cup stay in place?
A menstrual cup relies on light suction (and the strength of the surrounding vaginal muscles) to stay in place. Once inserted and released, the cup opens up and its rim creates a seal against the vaginal walls. This seal prevents leaks and keeps the cup from shifting.
To remove most menstrual cups, you must break the suction seal first by pinching the base. The Flex Cup works differently: its patented pull-tab stem is engineered to break the suction seal automatically as you pull, so removal never requires reaching up to pinch. This makes it easier for beginners and people with limited dexterity. As discussed in the IUD section below, it may also be a meaningful advantage for IUD users.
How are a period disc and cup inserted?
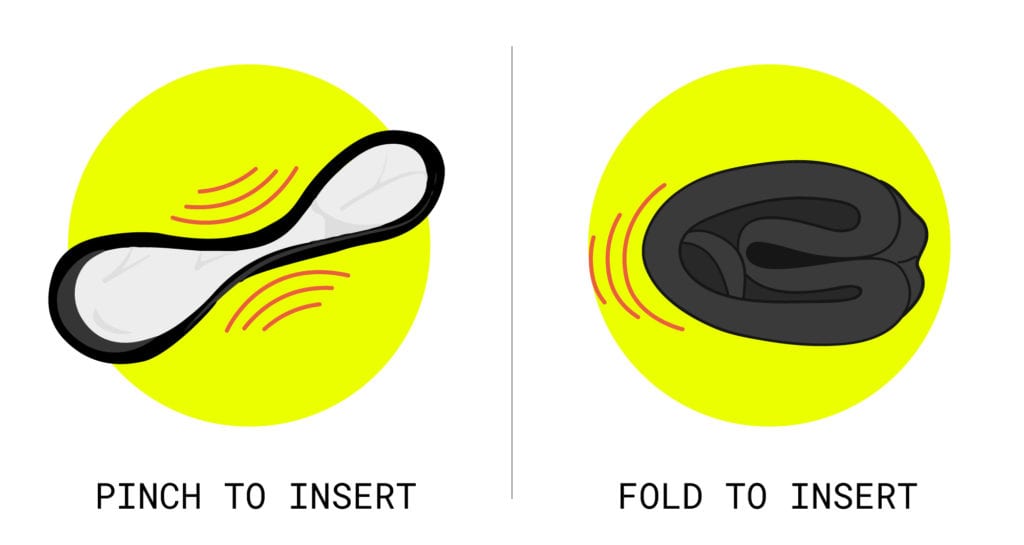
Inserting a menstrual disc starts with pinching it in half with the catch (the soft middle portion) facing down toward the floor so the disc looks like a bowl. Then, insert it into the vaginal canal: Use one finger to push it as far back as possible into the vaginal fornix so that the center is surrounding your cervix. To secure the disc in place, tuck the front rim behind the pubic bone.
Inserting a menstrual cup requires folding the cup (not just pinching) before insertion. Common folding techniques include the C-fold, the punchdown fold, and the 7-fold. The entire cup and stem must be placed inside of the vaginal canal. Once the cup is in a comfortable position, you verify the rim has fully opened and formed a circular seal against the vaginal walls. Some users gently rotate the cup to help it seal completely.
Both products have a learning curve. Research suggests that about three menstrual cycles is a typical familiarization phase, after which most users prefer their cup or disc to conventional products.
Video tutorial: How to insert Flex Disc & Flex Cup
Capacity: what does the research show?
If you have a heavy flow, capacity is probably near the top of your list, and this is where discs pull ahead. A 2023 study published in BMJ Sexual & Reproductive Health tested the blood capacity of 21 different period products and found that menstrual discs held the most of any product, averaging 61 mL. Tampons, pads, and menstrual cups all fell in the 20-50 mL range by comparison. 3
That same research also turned up something worth knowing about packaging claims: most products advertised higher capacity than lab testing actually confirmed, likely because manufacturers test with water rather than blood. So if you’ve ever wondered why a product felt like it needed changing sooner than the label suggested, that’s probably why.
For people who experience heavy menstrual bleeding (which affects roughly one in three people who menstruate), that extra capacity can make a real difference day-to-day. Both cups and discs can be worn for up to 12 hours, but on your heaviest days, a disc may simply mean fewer trips to the bathroom to change.
What are the disadvantages of menstrual discs?
Discs are a great option for many people, but they do have some drawbacks worth knowing about.
- Removal can be messier. Because a disc sits high in the fornix and holds a large volume, removal requires more care than a cup. You need to keep the disc level as you pull it out, which takes practice. Some people find removal easier in the shower, especially in their first few cycles.
- Fewer sizing options. Most disc brands offer one or two sizes, while the menstrual cup market has a wider range of sizes and firmness levels to suit different anatomies.
- Reusable discs have a shorter lifespan than cups. While a quality menstrual cup can last 5-10 years, most reusable disc brands recommend replacing every one to two years.
- The learning curve is real. Properly tucking the front rim behind the pubic bone takes practice, and an improperly placed disc is more prone to leaking.
That said, many people find that after a few cycles, discs become their preferred product, particularly because of their higher capacity, comfort, and period-sex compatibility.

Is it messy to remove a menstrual disc?
This is one of the most common questions people have before trying a disc for the first time, and it’s a fair concern. The answer: it can be, especially at first, but it doesn’t have to be.
Because a disc sits high in the vaginal fornix and collects a large amount of fluid, removal requires a steady hand and a bit of technique. The key is to keep the disc as horizontal as possible as you pull it out, rather than angling it upward. Most users find the process gets much tidier after the first one or two cycles. Removing your disc over the toilet helps, and some users prefer to do it in the shower while they’re learning.
One big advantage discs have here: the self-empty feature. Many users can empty their disc mid-wear without full removal (by bearing down while sitting on the toilet), which reduces how often you need to do a full removal during the day.
How do Flex Discs empty when you pee?
Flex Disc (and other menstrual discs) are sometimes said to “empty when you pee,” which can sound confusing. Here’s what’s actually happening.
When you’re sitting on the toilet and bear down (using your pelvic floor muscles, the same way you would when you’re urinating or to push during a bowel movement), the front rim of the disc can dip, allowing fluid to drain from the disc into the toilet. This is the “self-empty” feature.
This doesn’t happen automatically every time you urinate. It requires intentional bearing down, and the effect varies by person and anatomy. Some people find it works reliably; others don’t notice much difference. Either way, it’s a useful feature that many disc users appreciate on heavier days because it means fewer full removals throughout the day.
Menstrual discs vs. cups for period pain
Some people who experience menstrual cramps (or more severely, dysmenorrhea) report that menstrual discs feel more comfortable during their period than tampons or cups. The proposed reason: because a disc sits in the fornix rather than the vaginal canal, the vaginal walls are not constricted during wear, potentially allowing the uterus to contract with less resistance.
That said, large-scale clinical evidence specifically studying discs and pain reduction is still limited. If you experience significant dysmenorrhea, it’s worth discussing all of your options with a healthcare provider.
Can you have period sex with a disc or cup?
This is one area where discs and cups differ significantly:
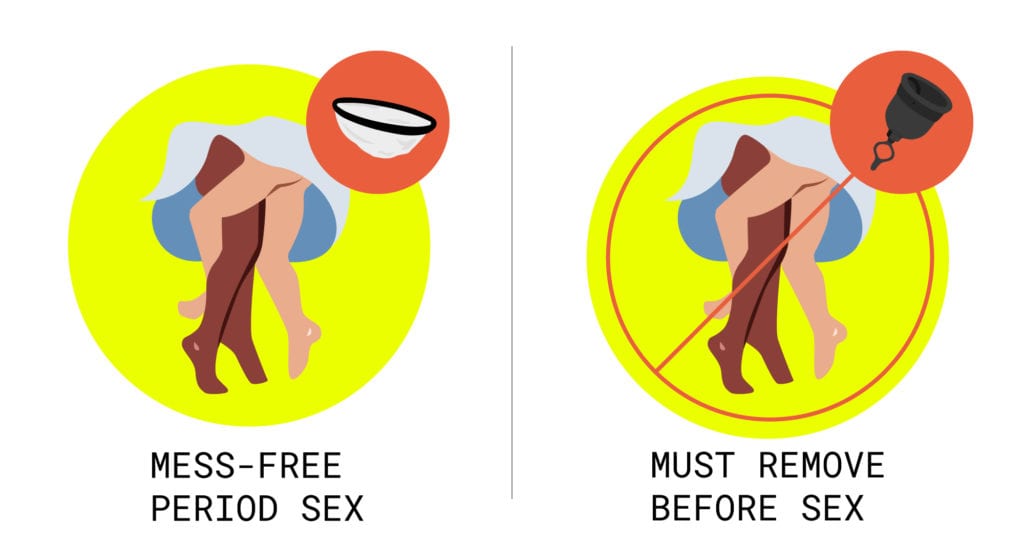
A menstrual disc does not occupy the vaginal canal. Because of its high, wide placement in the fornix, penetrative period sex is possible while wearing a disc, and most couples report neither partner can feel it during intercourse. This is one of the most cited reasons people switch from cups to discs.
A menstrual cup sits inside the vaginal canal and must be removed before penetrative sex.
Non-penetrative sex is perfectly compatible with either product.
Materials: what are menstrual discs and cups made from?
Disposable menstrual discs are made from medical-grade polymers, which are FDA-regulated materials used in many types of medical devices. The original Flex Disc uses a medical-grade polymer that softens slightly at body temperature, conforming to your anatomy.
Reusable menstrual discs and cups are typically made from 100% medical-grade silicone. Some brands use rubber or latex, so always check if you have sensitivities.
What makes these materials worth paying attention to is that they’re biologically inert, meaning they don’t interact with human tissue, don’t host harmful bacteria, and don’t disrupt your vaginal pH the way porous materials like cotton can. 4
This is one reason cups and discs are associated with a very low risk of toxic shock syndrome (TSS). A large 2019 analysis published in The Lancet Public Health reviewed 43 studies and data from over 3,000 people and found only five reported cases of TSS linked to menstrual cup use; an extremely rare occurrence by any measure. 5
Both Flex Cup and Flex Disc are FDA-registered, hypoallergenic, and free of BPAs, PFAs, phthalates, and natural rubber latex.
Reusability and sustainability
All menstrual cups are reusable. A well-maintained silicone cup can last anywhere from 5 to 10 years.
Menstrual discs are available in both formats:
- Reusable discs are made from medical-grade silicone and can last one to several years with proper care, depending on the brand.
- Disposable discs (like the original Flex Disc) are single-use.
If sustainability is your priority, both reusable cups and reusable discs are excellent options. Even single-use disposable discs create significantly less waste than conventional products, because you can wear a disc for up to 12 hours and use far fewer products per cycle than you would with tampons or pads.
Reusable cups and discs should be emptied and rinsed between uses, and boiled for 5-10 minutes at the end of each period cycle to fully disinfect them. For daily cleaning, use a mild, fragrance-free soap formulated for silicone (like Flex Foaming Cleanser) to avoid breaking down the material.
An important note for IUD users: disc vs. cup
If you have an IUD, this section is worth reading carefully before you choose a product. And before you make any switch, a conversation with your healthcare provider is always a good idea.
The main concern with menstrual cups and IUDs is suction. Because a cup creates a seal against the vaginal walls, there’s a possible association between cup use and IUD expulsion, AKA accidental self-removal. The research here is still evolving, but it’s substantial enough to take seriously.
A 2023 systematic review in Contraception and Reproductive Medicine looked at seven studies and found expulsion rates as high as 18.6% among cup users in some populations. A follow-up randomized trial published in Contraception in 2024 added more nuance: the elevated risk appeared most significant with one specific IUD frame type (the Nova-T), but not with the Paragard. This suggests that the shape of your IUD may matter as much as the product you’re using. 6
The Flex Cup may be a lower-risk option than standard menstrual cups for IUD users, precisely because of how its pull-tab works. Rather than requiring you to reach up and pinch the base to break the seal, the pull-tab does that automatically as you remove it. That means there’s far less suction force involved. Improper removal (pulling on a cup’s stem without breaking the seal first) is thought to be one of the main ways IUD displacement can happen, and the Flex Cup’s design reduces that risk.
Discs sidestep the suction question entirely, since they don’t use suction at all. A 2023 review in Obstetrics & Gynecology noted that no specific data yet exist on discs and IUD expulsion risk, but given the absence of suction, the theoretical risk is lower than with standard cups. That said, no clinical trials have confirmed this specifically, so it’s not a reason to skip the conversation with your doctor or Ob/Gyn.
If you have an IUD and are considering switching to a reusable internal period product, ask your Ob/Gyn which option makes the most sense for your specific IUD type and anatomy.

Sizing: does it matter?
Most menstrual discs come in one size; whereas menstrual cups may be available in multiple sizes depending on the brand.
Cup sizing is less about your internal dimensions and more about whether you’ve had a vaginal delivery. According to Ob/Gyn specialists, vaginal delivery may cause more laxity in the ligaments and a slightly wider vaginal opening, in which case a larger size is typically recommended. Otherwise, starting with the smallest size available is usually the right move.
If you have a dropped uterus, uterine prolapse, or a tilted uterus, a menstrual cup may not sit in place properly. A disc may be a more comfortable option in these cases, but always consult your provider first.
Menstrual disc vs. cup: side-by-side summary
| Menstrual disc (such as Flex Disc) | Flex Cup | Menstrual cup (generic) | |
| Placement | Vaginal fornix (at cervix) | Vaginal canal (below cervix) | Vaginal canal (below cervix) |
| Mechanism | Pubic bone support | Suction seal | Suction seal |
| Shape | Flat bowl/disc | Bell-shaped with pull-tab | Bell-shaped with stem |
| Capacity | Up to ~61mL (highest tested) | 20-50 mL | 20-50 mL |
| Wear time | Up to 12 hours | Up to 12 hours | Up to 12 hours |
| Reusable? | Reusable and disposable versions available | Always reusable | Always reusable |
| Period sex | Yes, disc stays in place | No, must be removed | No, must be removed |
| IUD caution | Lower theoretical risk (no suction) | Lower risk than standard cups (pull-tab removes without suction) | Yes, discuss with provider |
| Self-emptying? | Yes, mid-wear emptying possible | No, must remove to empty | No, must remove to empty |
| Removal ease | Moderate learning curve | Pull-tab breaks seal automatically; removes like a tampon | Requires pinching to break seal |
| Learning curve | Yes (~3 cycles) | Yes (~3 cycles) | Yes (~3 cycles) |
| Flex product | Flex Disc / Flex Reusable Disc | Flex Cup | N/A |
Key takeaways: How to decide between a cup and a disc
Choose Flex Disc or Flex Reusable Disc if you:
- Have a heavy flow and want maximum capacity
- Want to have mess-free penetrative period sex
- Prefer a product with no suction
- Have an IUD
- Want both reusable and disposable options
Choose Flex Cup if you:
- Prefer a product similar in placement to a tampon
- Want the easiest possible removal (the pull-tab does the work)
- Have an IUD and want a cup option with reduced suction risk
- Are a first-time internal period product user
Both options provide up to 12 hours of protection, are made with body-safe, non-toxic materials, and are a meaningful upgrade from conventional disposable products for your wallet, your body, and the environment.
If you have any medical conditions (including pelvic floor dysfunction, an IUD, endometriosis, or other pelvic concerns) it’s always a good idea to speak with your healthcare provider before making the switch.
Have questions about Flex Cup, Flex Reusable Disc, or Flex Disc? Our Flexperts are always here to help. Email us at hello@flexfits.com.
This article is informational only and is not offered as medical advice, nor does it substitute for a consultation with a physician.
- Samuelson Bannow, B. et al. (2023). Red blood cell capacity of modern menstrual products: considerations for assessing heavy menstrual bleeding. BMJ Sexual & Reproductive Health. doi:10.1136/bmjsrh-2023-201895[↩]
- Madar, J., Gaucher, M., Barbaroux, A., et al. (2024). Risks of urogenital infections and expulsion associated with the combination of an IUD and a menstrual cup. Gynécologie Obstétrique Fertil Sénologie, 52(12), 683–689. doi:10.1016/j.gofs.2024.07.003[↩]
- Blumenthal, P. et al. (2023). Going with the flow: the emergence of menstrual science [Editorial]. BMJ Sexual & Reproductive Health. doi:10.1136/bmjsrh-2023-201972[↩]
- Rao, H. M., Rajkumar, K., Narayana, V., Akash, M., Sabu, J., & Ramadoss, R. (2022). Bioinert and bioactive materials – narrative review. Journal of Pharmaceutical Negative Results, 13(Special Issue 7), 2251–2255. https://doi.org/10.47750/pnr.2022.13.S07.309[↩]
- van Eijk, A.M., Zulaika, G., Lenchner, M., et al. (2019). Menstrual cup use, leakage, acceptability, safety, and availability: a systematic review and meta-analysis. The Lancet Public Health, 4(8), e376–e393. doi:10.1016/S2468-2667(19)30111-2[↩]
- Bowman, N. & Thwaites, A. (2023). Menstrual cup and risk of IUD expulsion: a systematic review. Contraception and Reproductive Medicine, 8(1), 15. doi:10.1186/s40834-022-00203-x[↩]