Ask an OB/GYN: What’s that lump inside my vagina?
Everything you need to know about what goes bump in the night.
And by the night, we mean your vagina. Nobody wants to be going through their day—wiping, masturbating, changing their Flex disc—only to suddenly, alarmingly feel a lump in their vagina.
It’s possible the bump or lump is just a part of your anatomy you’re noticing for the first time…or it may be a more recent development. Either way, you probably want to know what it is, why you have it, and what you can do about it.
We had board-certified gynecologist and Flex® medical advisor Dr. Jane Van Dis, answer a few of the first questions that might send you scrambling for the nearest search engine when you find a lump in your vagina.
What’s that lump in my vagina!?
First of all: don’t panic. I know finding a lump on your genitals can be alarming, but keep in mind that every vagina is different—they have different folds, ridges, bumps, and lumps. What you’ve found may simply be a natural part of your anatomy. Even if it’s not, vaginal lumps are surprisingly common and often harmless.
Before we go further, it’s worth clarifying a few terms. We often use “vagina” as a catchall for a region that deserves a bit more specificity—feel free to skip this section if you’re intimately familiar with the anatomy of your genitalia.
- Vagina: The vagina itself is actually just the interior muscular canal, which extends from the cervix to the opening of the vagina. It’s part of your internal genitalia, along with the uterus, cervix, uterine tubes, and ovaries.
- Vulva: The vulva refers to all of the external genitalia: vaginal lips (the labia minora and majora), mons pubis, clitoris, urethra, vaginal opening, Bartholin’s glands, and a few other structures.
Now that we’re on the same page…if you’ve found a lump in your vagina (not your vulva), it could be a few different things.
Vaginal Cysts
The most likely culprit behind a bump or lump in your vaginal area, a vaginal cyst is a small projection found on the lining of the vagina. They’re typically no larger than the size of a pea and are rarely painful. Different types of vaginal cysts fall into a few categories:
- Vaginal Inclusion Cysts → Very common, this type of cysts develop in response to trauma or injury (like childbirth) and they are most likely to be found at the base (or bottom) of the vagina.
- Bartholin’s Cysts →Also relatively common, these lumps near the vaginal opening can form on either one or both sides (I’ll get into more detail below).
- Gartner’s Duct Cysts → Generally only associated with pregnancy.
- Endometriosis Cysts → Small cysts formed from lumps of endometrial-type tissue.
Pressure From an Adjacent Organ
A less likely explanation for a vaginal lump, though one that becomes more common with age. Sometimes the uterus, rectum, or bladder can press against the vaginal wall, causing a bump or lump to form. Or, quite commonly, hard poop in your rectum can feel like a bump in your vagina.
Can a lump in the vagina be cancerous?
Also rare, though again, more common in those over 40. Vaginal cancer can cause lumps to grow inside the vagina, which might require any number of treatments based on the stage of progression. Not all vaginal lumps are cancerous. They can be caused by non-cancerous conditions like cysts or infections.
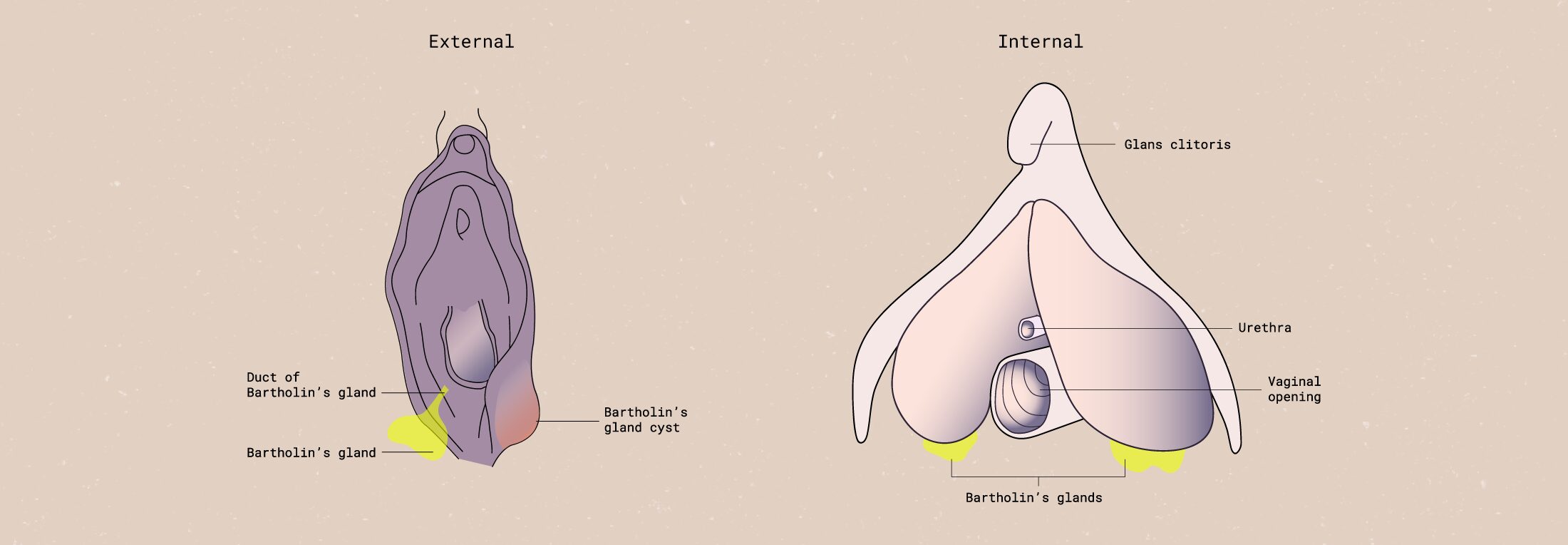
What is a Bartholin cyst?
As one of the more common types of vaginal cysts, it can be useful to have a clearer understanding of what, exactly, a Bartholin gland cyst is.
The Bartholin’s glands provide lubrication (wetness) to the vagina; when the opening to the glands gets blocked, fluid builds up. This creates a fluid-filled sac that can form on—you guessed it—your Bartholin gland, located on both sides of your vaginal opening.
What causes Bartholin Cysts?
Bartholin’s cysts can occur as a response to an injury or irritation in the area, a Sexually Transmitted Infection (STI), or a bacterial infection. No one knows why, exactly, but some women are simply predisposed to getting them. They aren’t usually contagious, though of course, if you get one as a result of an STI, the STI is.
Symptoms of Bartholin’s cysts include discomfort or pain during sexual intercourse, walking, wiping, inserting menstrual products, or even sitting. Thankfully, they often clear up on their own within a few weeks. However, if you notice any signs of infection of a cyst—drainage, fever, tenderness, fluid or collection of pus—you should get a professional assessment.


What if the lump is near my vagina, not in it?
If you’ve discovered a lump or bump outside your vagina, somewhere on your vulva or the surrounding skin, there are any number of additional explanations. Some possibilities include:
- Skin irritations
- Herpes infection
- Syphilis infection
- HPV or condyloma infection (genital warts)
- Molluscum Contagiosum (viral infection)
- Chlamydia
- Ingrown hairs
- Pimples
- Fordyce spots
- Varicosities
- Skin tags (tissue that forms after injury, most commonly)
- Allergic rashes
And because your mind almost certainly went there right away: yes,lumps inside the vagina or on the vulva may also be signs of an STD. Different STDs generally produce distinct bumps, from the small blisters of Herpes to the cauliflower-like clusters of genital warts caused by HPV.
How worried should I be if I find a lump in my vagina?
Almost everyone will get a vaginal lump at some point in their lives. Genital skin is sensitive; occasional bumps are common, often innocuous, and many resolve without issue all on their own. However,it’s always best to have any lump looked at by a gynecologist, which allows for identification and treatment—as well as possible biopsy or testing—in order to determine the exact cause.
Sometimes, a lump may be a little larger or more tender, or you might notice it growing in size. In these cases, you can try a few at-home approaches before your appointment with your gynecologist to help it resolve as quickly and painlessly as possible:
- Sitz baths.
- To help with discomfort, promote healing, and encourage a cyst to drain on its own, you can take a sitz bath. Just sit in a bathtub with a few inches of warm water a few times a day for several days. Alternatively, you can try a warm compress.
- Take OTC pain relievers.
- Over-the-counter pain medicine can help manage any pain or discomfort you may be feeling.
- Let your genitals breathe.
- Avoid wearing tight clothing or synthetic fibers. Instead, practice good hygiene and wear loose clothes and cotton underwear to keep things clean and dry.
- Avoid unnecessary friction.
- No tampons, and (unfortunately) no sex, which might irritate any lumps or bumps.
Never try to squeeze or drain a lump on your own—it will only increase the likelihood of spreading the infection and risk complications. I also still recommend talking to your doctor first whenever you discover a vaginal bump or lump; any changes in your body should always be brought to the attention of a healthcare professional.
Do I need to see a doctor?
The short answer: yes. Though lumps and bumps are common, I always advise patients to come to me for an exam to ensure everything’s shipshape. In general, if you have a lump that doesn’t resolve on its own within a week or two—especially if you’re over 40—make time to see your healthcare provider.
Typically, your OB/GYN will perform a physical exam to help determine the nature of your lump and look for signs of infection. They may also request imaging tests, swab the area to test for bacterial or sexually transmitted infections (STIs), or call for a biopsy to rule out cancer.
If you have an infected vaginal cyst, a doctor may prescribe antibiotics, surgical draining of the cyst, or—in the case of those with recurring Bartholin’s cysts— remove the gland entirely as a treatment option.
Again, when in doubt, see a doctor. And don’t be embarrassed! The more honest you are, the better we’re equipped to help.
Lump in Vagina: Takeaways
- The vagina is the muscular canal between your vaginal opening and cervix.
- Lumps and bumps in your vagina are common.
- They’re often small, painless cysts and not a cause for alarm
- However, if a lump persists for over a week, is large, becomes painful, becomes infected or if you notice changes in the size of the cyst, see your OB/GYN.
- Even if your lump isn’t painful, seeing a doctor is a good idea—especially if they’re recurring or you’re over the age of 40.
- Seeing a professional sooner rather than later can help address symptoms quickly and reduces the risk of complications.


This article is informational only and is not offered as medical advice, nor does it substitute for a consultation with your physician. If you have any gynecological/medical concerns or conditions, please consult your physician.
© 2024 The Flex Company. All Rights Reserved.